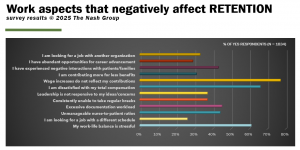
Bridging the Healthcare Disconnect: Why Labor Management Needs a People-Focused Approach
The healthcare industry prides itself on its dedication to patient well-being, yet a critical disconnect in labor management practices threatens to undermine this very mission. Outdated approaches, a reliance on …