Analyzes Medicaid enrollment and spending trends for FY 2020 and FY 2021 based on data provided by state Medicaid directors as part of the 20th annual survey of Medicaid directors in all 50 states and the District of Columbia. Overall, 43 states2 responded to the survey by mid-August 2020, although response rates for specific questions varied. The methodology used to calculate enrollment and spending growth as well as additional information about Medicaid financing can be found at the end of the brief. Key findings include the following:
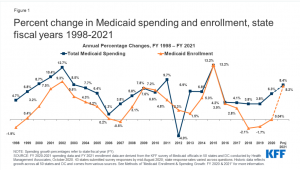
- After relatively flat enrollment growth in FY 2020 (0.04%), states responding to the survey expect Medicaid enrollment to jump in FY 2021 (8.2%) attributed to the FFCRA’s MOE requirements and to the economic downturn that started late in FY 2020.
- Across all reporting states, states were anticipating that total Medicaid spending growth would accelerate to 8.4% in FY 2021 compared to growth of 6.3% in FY 2020. Enrollment was the primary factor identified as putting upward pressure on expenditure growth in FY 2021.
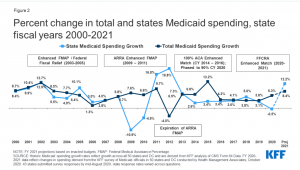
- While expected state spending on Medicaid is crucial to state budgets, the projections in this year’s survey do not provide a clear picture because enhanced federal funding is now slated to expire at the end of March 2021 based on the recent renewal of the Public Health Emergency (PHE), later than states had generally assumed. At the time of the survey, states estimated that state Medicaid spending would decline in FY 2020 (-0.5%) and then sharply increase in FY 2021 (12.2%) with most states assuming that the enhanced matching funds would expire by December 2020.
- Looking ahead, states are faced with many layers of uncertainty about the trajectory of the pandemic and economic downturn as well as the duration of the enhanced FMAP and the outcome of the elections in November.
source: https://www.kff.org/medicaid/issue-brief/medicaid-enrollment-spending-growth-fy-2020-2021/