The cost of hospital admission for patients with the coronavirus can top tens of thousands of dollars, and there have been hundreds of thousands of hospitalizations just in the early months of the pandemic. However, social distancing measures, concerns over hospital capacity, and fears of contracting the virus are leading to some other healthcare being delayed or forgone. On net, it is not yet clear how these upward and downward cost pressures will balance out in 2020 and 2021.
This chart collection summarizes what is known so far about how health costs and utilization have changed during the pandemic.
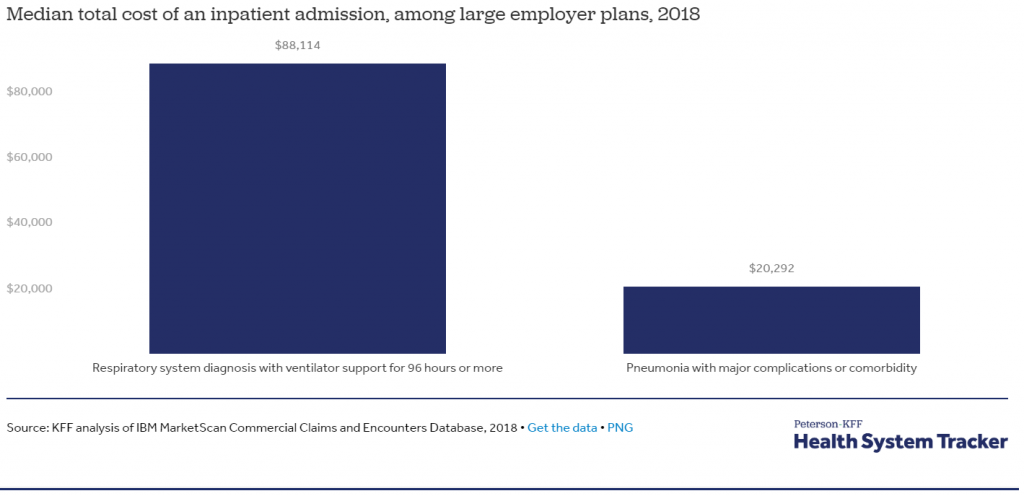
1- An inpatient admission for COVID-19 treatment could top tens of thousands of dollars: Based on an analysis of spending by large employer plans for respiratory diagnoses, KFF found hospitalization costs exceed $20,000 for pneumonia patients with complications and more than $80,000 for patients with the most serious respiratory conditions that required ventilator support. For people with employer coverage, most of these costs would be paid by the plan, but out-of-pocket costs could exceed $1,300.
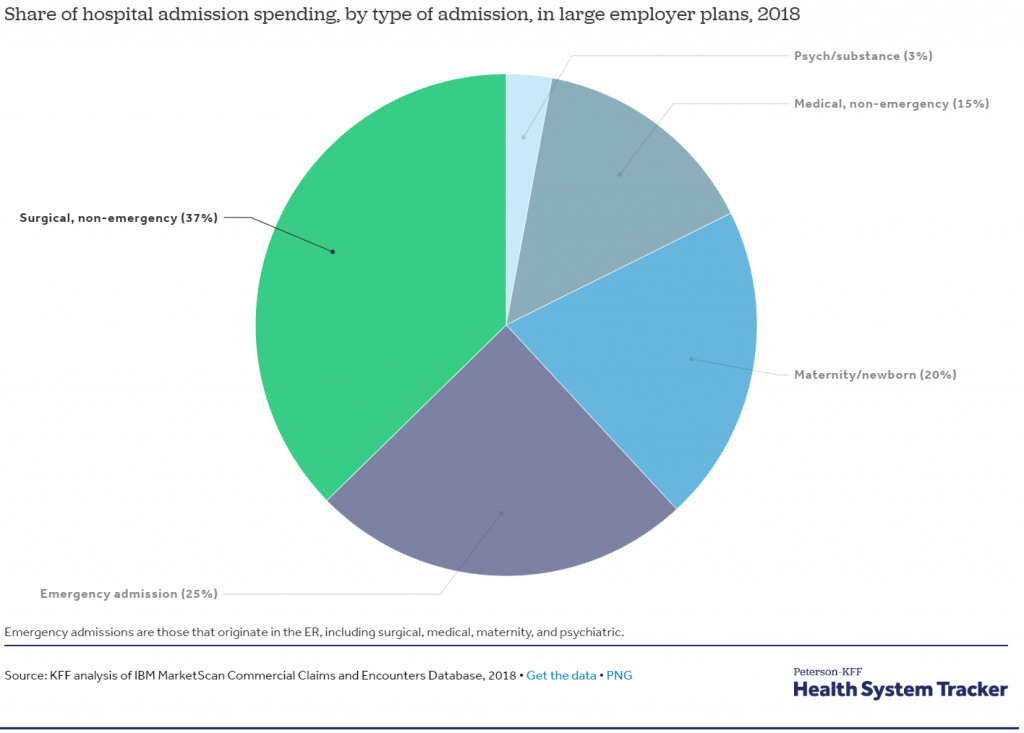
2- Elective procedures, most of which have been postponed during shelter-in-place, are typically a substantial share of spending at hospitals: Many hospitals across the country canceled or postponed elective surgeries to allow more capacity for treating COVID-19 patients. KFF analyzed claims data from non-elderly enrollees of large employer plans. In 2018, 37% of hospital admission spending by large employer plans was on surgical procedures that did not originate in the emergency room, some of which may be delayed or foregone.
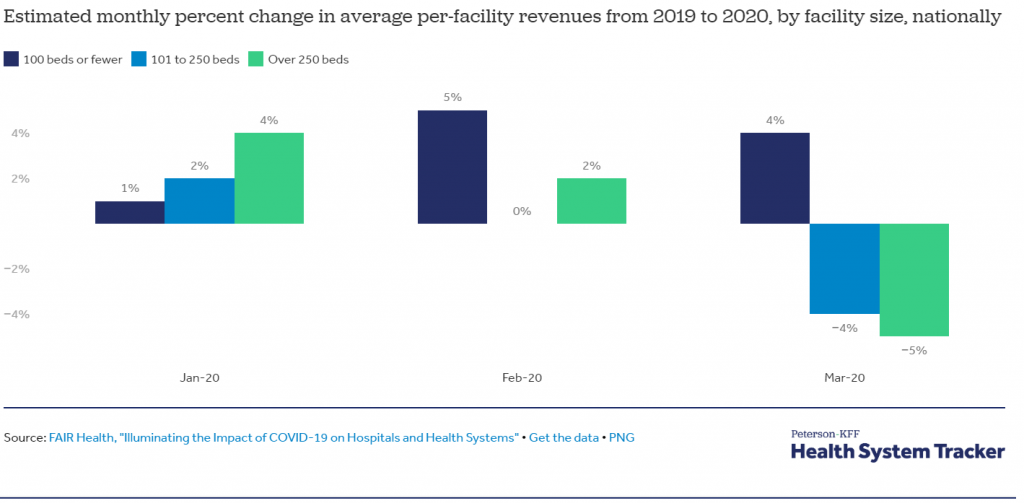
3- Many hospitals lost revenue in March, amid social distancing measures and cancellations of elective procedures: Following social distancing efforts and cancellations of elective procedures in March 2020, many hospitals began losing revenue. FAIR Health analyzed private insurance claims submitted by hospitals and health systems from January through March of 2020 to the same time period in 2019, finding that nationally, midsize and large facilities began seeing a decrease in revenues in March. On average, hospitals in the northeastern U.S. (including small hospitals) saw sharper drops in revenue during March, according to the analysis. As discussed below, there are some indications that health care utilization may have begun to pick back up in late April and early May.
Additional charts can be found in this KFF report.